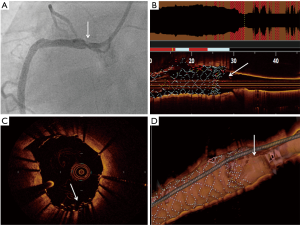
Stent accordion phenomenon visualized with optical coherence tomography
Percutaneous coronary intervention (PCI) was done in a 57-year-old male with chronic kidney disease who presented with non-ST segment elevation myocardial infarction. Coronary angiogram showed two vessel disease of the left anterior descending artery (LAD) and the right coronary artery (RCA). The LAD was successfully stented. After predilatation and rotablation, PCI was performed with 2 overlapping drug eluting stents (DES) Promus (Boston Scientific, Marlborough, Massachusetts, USA) 3 mm × 38 mm to the mid RCA and Resolute Onyx 3.5 mm × 34 mm (Medtronic, Minneapolis, Minnesota, USA) to the ostial proximal segment, respectively. After post dilatation using a 3.5 non-compliant balloon, there was a stenotic segment at the ostial area where the stent was implanted (white arrowhead Figures 1,2). The patient was asymptomatic and no changes in the electrocardiogram were noted. However, the ostial stenosis did not resolve despite administration of intracoronary nitrates. Optical coherence tomography showed longitudinal deformation/compression of the ostial RCA stent (white arrowhead Figures 1B,3). Some of the proximal stent struts were well apposed but is visualized alongside distorted and crumpled malapposed stent struts (white arrowhead Figures 1C,3). Despite prior ostial stent deployment, there was a stenosis at the ostial area right before the guide catheter and no stent struts can be visualized on three-dimensional rendering (white arrowhead Figure 1D). The deformed portion of the ostial RCA was stented further with a DES (Ultimaster 4.0 mm × 12 mm, Terumo, Shibuya, Tokyo, Japan). Postdilatation was completed with 4.0 non-compliant balloon and adequate stent expansion and apposition was achieved. Patient was maintained on dual antiplatelet therapy and the rest of the hospital stay was unremarkable.


Longitudinal stent deformation or the accordion phenomenon is an unusual but increasingly recognized complication after percutaneous catheter interventions, characterized by mechanical distortion or shortening of a stent in the longitudinal axis after deployment. Data from the U.S. Food and Drug Administration (FDA) Manufacturer and User Facility Device Experience (MAUDE) database revealed an occurrence of 0.2% in a span of 4 years (3). Other names such as concertina-like, pseudofracture, pseudostenosis and crumpling have been used synonymously to describe its characteristic appearance. It should be suspected angiographically by the appearance of new onset stenosis after stent deployment that can be sometimes mistaken for spasm and is persistent despite nitroglycerin administration. In our case the accordion phenomenon may have been caused by the interaction of the guiding catheter and stent deployed in the aorto-ostial position. It is possible that stents that are relatively undersized after initial deployment are subsequently ‘caught’ and distorted by secondary equipment that is passed into the coronary vessel with compression of the proximal edge of ostially placed stent with the guide catheter (4). It can be also induced by lesion complexity, secondary PCI equipment such as guidewires as well as the inherent mechanical properties of the stent itself (5). With regards to the stent platform, results of bench studies indicate that stent longitudinal strength, defined as the resistance to shortening or elongation, appears to be related to the number of connectors between hoops. With the newer generation DES, there is a trade-off between number of connectors for longitudinal strength at the expense of stent flexibility (6). Furthermore, it was noted that stents with 2-link offset peak-to-peak design are those that are most prone to compression (7). Despite being a rare event, recognition is of paramount importance as this area of deformation may be predisposed to potential catastrophic complications such as stent thrombosis (8). Careful examination on fluoroscopy as well as additional imaging modalities such as optical coherence tomography and intravascular ultrasound may be necessary for diagnosis as well as to guide treatment decisions (9). Treatment consists of cautious post dilation across the damaged portion of the stent as well further optimization of deployment of a second stent (10). This case emphasizes the importance of PCI operators being meticulous in the conduct of their procedure, such as proper angiographic recognition, complete understanding of stent design characteristics that will influence the choice of stent selected for deployment, careful manipulation of guiding catheter, and achievement of optimal stent apposition.
Acknowledgements
Dr. Yeo has received research funding from Medtronic and honoraria from Abbott Vascular, Boston Scientific, Amgen and Menarini.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Cuenza LR, Yeo KK. Coronary Angiogram left anterior oblique view showing a stenotic area at the ostial segment after stent placement. Asvide 2017;4:561. Available online: http://www.asvide.com/articles/1880
- Cuenza LR, Yeo KK. Optical coherence tomography pullback short axis and long axis views confirming longitudinal stent deformation at the ostium. Asvide 2017;4:562. Available online: http://www.asvide.com/articles/1881
- Williams PD, Mamas MA, Morgan KP, et al. Longitudinal stent deformation: a retrospective analysis of frequency and mechanisms. EuroIntervention 2012;8:267-74. [Crossref] [PubMed]
- Mamas MA, Williams PD. Longitudinal stent deformation: insights on mechanisms, treatments and outcomes from the Food and Drug Administration Manufacturer and User Facility Device Experience database. EuroIntervention 2012;8:196-204. [Crossref] [PubMed]
- Guler A, Guler Y, Acar E, et al. Clinical, angiographic and procedural characteristics of longitudinal stent deformation. Int J Cardiovasc Imaging 2016;32:1163-70. [Crossref] [PubMed]
- Ormiston JA, Webber B, Webster MW. Stent longitudinal integrity bench insights into a clinical problem. JACC Cardiovasc Interv 2011;4:1310-7. [Crossref] [PubMed]
- Prabhu S, Schikorr T, Mahmoud T, et al. Engineering assessment of the longitudinal compression behaviour of contemporary coronary stents. EuroIntervention 2012;8:275-81. [Crossref] [PubMed]
- Rigattieri S, Sciahbasi A, Loschiavo P. The clinical spectrum of longitudinal deformation of coronary stents: from a mere angiographic finding to a severe complication. J Invasive Cardiol 2013;25:E101-5. [PubMed]
- Abdel-Hadi H, Shah AH, Džavík V. Role of Optical Coherence Tomography in the Assessment of Stent Deformation. Can J Cardiol 2016;32:396.e1-2. [Crossref] [PubMed]
- Noad RL, Hanraty CG, Walsh SJ. Clinical Impact of Stent Design. Interventional Cardiology Review 2014;9:89-93. [Crossref]


