
Two-dimensional speckle tracking of the abdominal aorta: a novel approach to evaluate arterial stiffness in patients with Turner syndrome
Introduction
Turner syndrome (TS) is a chromosomal disease characterised by the complete or partial absence of one of the two X chromosomes in females (1). Approximately one in 2,500–3,000 female newborns is affected by this disorder (1). TS is associated with multiple cardiometabolic and cardiovascular risk factors such as diabetes, arterial hypertension, lipid anomalies and overweight, resulting in an elevated risk for arteriosclerosis, even in young age (2,3). Moreover, congenital heart defects like bicuspid aortic valve or aortic coarctation can be found more frequently in girls and women with TS (3,4). The early detection as well as the regular monitoring of vascular impairments is essential for the overall outcome in these patients (5).
Arterial stiffness is considered to be a reliable cardiovascular risk factor (6). Recent studies could demonstrate an increased arterial stiffness in TS patients (7-9). During echocardiographic examination, M-Mode of the abdominal aorta is commonly used to asses arterial stiffness by putting maximal and minimal aortic expansion in relation (10). However, M-Mode is limited by its one-dimensional image acquisition (10). Due to the complexity of aortic anatomy and physiology, modern sonographic techniques must overcome this limitation to evaluate arterial stiffness more accurately.
In 2008, Oishi et al. described a novel approach to asses arterial stiffness of the abdominal aorta using two-dimensional speckle tracking (2DST) (10). In short, this technique fixes on various aortic sonographic pixels also called “speckles” and “tracks” them two-dimensionally over space and time. For each speckle, a strain value is calculated describing its percentage in deformation (11). Strain values are then averaged into a mean strain of the abdominal aorta (11). The stiffer the vessel, the lower its deformation and therefore the lower its strain.
Non-invasiveness and angle independency make 2DST an interesting screening tool to assess abdominal aortic stiffness during echocardiographic routine examination in patients with TS. To the best of our knowledge, 2DST of the abdominal aorta has not been performed yet in TS subjects.
The aim of this study was (I) to investigate whether 2DST of the abdominal aorta detects vascular impairments in patients with TS and (II) whether this technique might be applicable as a screening tool for arterial stiffness during echocardiographic examination.
Methods
Ethical statement
This study was a retrospective analysis of prospectively collected data and was approved by the Ethics Committee of the Ärztekammer des Saarlandes (State Chamber of Physicians of the German federal state of Saarland), Faktoreistraße 4, 66111 Saarbrücken, Germany, on March 23rd, 2018; approval statement No. 07/18. Prior written informed consent was obtained from all patients or the parents or legal guardians of patients under legal age.
Study population
Thirty-five patients with a confirmed genetic diagnosis of TS and 19 healthy age-matched controls were recruited for this study between November 2016 and April 2018. TS patients who were seen regularly at the departments of pediatric cardiology and pediatric endocrinology of Saarland University Hospital were selected. In collaboration with the German Turner Syndrome Association (Turner-Syndrom-Vereinigung Deutschland e.V.), additional external TS patients were recruited into our study. The control group consisted of healthy age-matched volunteers and patients with accidental heart murmurs in whom cardiac pathologies had been excluded by echocardiography and electrocardiography. Body surface area (BSA, m2) was calculated according to Mosteller’s formula (12).
Echocardiographic examination was carried out using a 2.5–3.5 MHz phased array transducer with a Vingmed Vivid 9 ultrasound system (General Electrics Healthcare, Fairfield, CT, USA).
Echocardiographic assessment of the left ventricular function
Left ventricular dimensions
Left ventricular dimensions were assessed at the tip of the mitral valve in parasternal long axis view using M-Mode echocardiography. Myocardial borders were marked in end-diastolic (QRS complex in ECG) and end-systolic (end of T-wave in ECG) phase. The following parameters were measured: interventricular septum thickness at end-diastole (IVSd, cm), interventricular septum thickness at end-systole (IVSs, cm), left ventricular internal dimension at end-diastole (LVIDd, cm), left ventricular internal dimension at end-systole (LVIDs, cm), left ventricular posterior wall thickness at end-diastole (LVPWd, cm), left ventricular posterior wall thickness at end-systole (LVPWs, cm), left ventricular end-diastolic volume (EDV, mL), left ventricular end-systolic volume (ESV, mL), stroke volume (SV, mL), ejection fraction (EF, %), fractional shortening (FS, %), left ventricular end-diastolic mass (LV Mass, g). To ensure better comparability of left ventricular morphometric data between TS patients and controls, “Z scores of cardiac structures” were calculated according to Pettersen et al. for the following parameters: IVSd, IVSs, LVIDd, LVIDs, LVPWd, LVPWs (13). Moreover, EDV, ESV, SV and LV Mass were put in relation to BSA.
Left ventricular diastolic function
Left ventricular diastolic function was evaluated at the tip of the mitral valve through pulsed Doppler echocardiography. Mitral inflow peak velocities were recorded at early (E peak velocity, cm/s) and late (A peak velocity, cm/s) diastole. The ratio of E/A was calculated.
Left ventricular systolic deformation
Left ventricular systolic deformation was assessed through 2DST echocardiography. The left ventricle was recorded in apical two chamber view, apical three chamber view and apical four chamber view, using a frame rate of 60–90 fps. The recorded clips were then analysed offline on a separate work station (EchoPAC PC version 202, General Electrics Healthcare). The endocardium was marked thoroughly, and the region of interest was precisely adjusted to the thickness of the myocardium. End-systole was defined as the point of aortic valve closure. Mean peak systolic strain was calculated subsequently by the software for the apical chamber view (GLPS_A2C, %), the apical three chamber view (GLPS_LAX, %) and the apical four chamber view (GLPS_A4C, %). Furthermore, an average of GLPS_A2C, GLPS_LAX and GLPS_A4C was calculated and defined as GLPS_AVG (%).
M-Mode of the abdominal aorta
The abdominal aorta was recorded in long subxiphoid view at epigastric level using a 2.5-3.0 MHz phased array transducer with a Vingmed Vivid 9 ultrasound system (General Electrics Healthcare). Recorded clips where then analyzed offline. Maximal (Dmax, mm) and minimal (Dmin, mm) abdominal aortic diameters were measured manually on a separate work station (EchoPAC PC version 202, General Electrics Healthcare). M-Mode assessed abdominal aortic strain (AAO-S, %) was defined as

2DST of the abdominal aorta
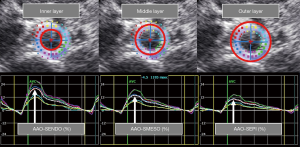
Basic methodological ideas of abdominal aortic 2DST were inspired by Oishi et al. (10). The abdominal aorta was recorded in short subxiphoid view at level of epigastrium using a 2.5–3.0 MHz phased array transducer with a Vingmed Vivid 9 ultrasound system (General Electrics Healthcare) over three consecutive cardiac cycles. A frame rate of 60–90 fps was applied. Acquired clips were subsequently analysed offline on a separate work station (EchoPAC PC version 202, General Electrics Healthcare). Notably, this work station was originally designed to measure myocardial deformation. Mean peak circumferential strain of the abdominal aorta (AAO-S, %) was measured semi-automatically through the software’s function “SAX-AP” by marking the aortic endothelia thoroughly. The width of the region of interest was adjusted to the smallest possible setting (diameter) to ensure tracking of the abdominal aortic wall only and to prevent speckles from tracking para-aortic tissue. AAO-S was then identified manually within the strain-diagram and displayed the mean curve’s maximum. The procedure was executed for single layers of the abdominal aorta, resulting in a mean peak circumferential strain of the inner (AAO-SENDO, %), middle (AAO-SMESO, %) and outer abdominal aortic layer (AAO-SEPI, %) (Figure 1). 2DST of the abdominal aorta was carried out three times for each layer and an average was then calculated. In addition, we divided AAO-SENDO, AAO-SMESO and AAO-SEPI by Dmax (AAO-SENDO/Dmax, AAO-SMESO/Dmax, AAO-SEPI/Dmax, % per mm).
Arterial distensibility
Arterial distensibility (mmHg−1×10−3) was defined as
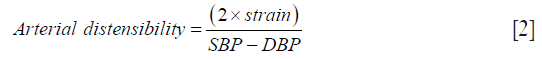
and was calculated separately for M-mode and for AAO-SMESO (14). SBP represents the systolic brachial blood pressure and DBP the diastolic brachial blood pressure in mmHg.
Pulse wave velocity (PWV) and blood pressure measurement
PWV (m/s) was measured through an automatic oscillometric blood pressure measuring device (Mobil-O-Graph, I.E.M. GmbH, Stolberg, Germany). The Mobil-O-Graph determines PWV mathematically through brachial pressure waveforms (15). Its accuracy of PWV assessment has been validated through invasive intra-aortic catheter measurements (16). Moreover, PWV reference values for healthy children and adults are published in literature for this specific device (17,18). Before starting the PWV examination, study participants were asked to rest in a seated position for at least 5–10 minutes. Brachial systolic (SBP, mmHg) and diastolic blood pressure (DBP, mmHg) were measured using a conventional blood pressure monitor (CARESCAPE V100 Monitor, General Electrics Healthcare). Cuff sizes were selected according to the left upper arm circumference.
Statistical analyses
Statistical analyses were performed utilizing SPSS 24 (Released 2016. IBM SPSS Statistics for Windows, Version 24.0. IBM Corp., Armonk, NY, USA). All continuous variables were tested for normality using the Kolmogorov–Smirnov test. Data are shown as mean ± SD or as median, minimum and maximum if not normally distributed. Continuous variables with normal distribution were compared using the independent-samples t-test. The Mann-Whitney U test was used to compare non-normally distributed continuous variables. Correlations were analysed using the Pearson correlation for normally distributed variables or the Spearman correlation for non-normally distributed variables. A P value <0.05 was considered statistically significant. Relative intra- and interobserver variability was assessed by two experienced investigators for AAO-SENDO, AAO-SMESO and AAO-SEPI in ten randomly selected study subjects. Relative intra- and interobserver variability was defined as
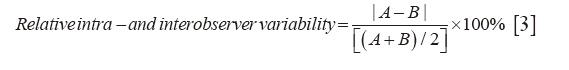
Results
Patient characteristics
In total, 35 patients with TS and 19 heathy age-matched subjects were prospectively recruited for this study. Median age was 16.58 years in the TS group and 16.35 years in the control group. No significant difference existed in age between the two groups. Except for one boy with a rare form of mosaic TS, both groups consisted exclusively of females. TS patients were significantly smaller in height and had a significantly lower BSA (m2). Body mass index (BMI, kg/m2) was significantly higher in TS patients. Compared to controls, TS patients showed a significantly higher heart rate (bpm). No significant differences in SBP and DBP was observed between both groups. The patient characteristics are summarized in Table 1.
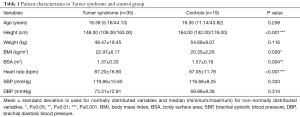
Full table
Karyotype and cardiovascular morbidity in TS patients
Out of 35 TS patients, 19 (54.3%) had monosomy X (45, X0), while 11 (31.4%) had a mosaic form of TS. Two (5.7%) TS patients had a structural chromosomal aberration of an X chromosome. Three (8.6%) patients were diagnosed as having “Turner syndrome, unspecified (Q96.9)”.
In total, 14 (40.0%) patients with TS presented with congenital heart defects. Nine (25.7%) patients had a bicuspid and two (5.7%) had a monocuspid aortic valve. Three (8.6%) patients showed a significant dilatation of the ascending aorta. Five (14.3%) patients were diagnosed with coarctation of the aorta. Four (11.4%) patients underwent cardiac surgery, primarily to correct coarctation of the aorta. Three (8.6%) patients had partial anomalous pulmonary venous drainage. Of note, some TS patients displayed multiple heart defects. Five (14.3%) patients had hypertension and were on anti-hypertensive medication, eight (22.9%) were overweight and six (17.1%) were obese. Three (8.6%) patients demonstrated disorders of carbohydrate metabolism. Seventeen (48.6%) patients were receiving growth hormone therapy during study participation. Overall, 18 (51.4%) patients were receiving estrogen hormone therapy and another 11 (31.4%) thyroid hormone therapy during study participation.
Echocardiographic assessment of the left ventricular function
Left ventricular dimensions
No significant differences were assessed in left ventricular dimensions between TS patients and controls. Detailed results of left ventricular dimensions are presented in Table 2.
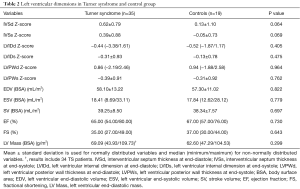
Full table
Left ventricular diastolic function
No significant difference was detected in the E peak velocity between the TS and the control group (mean ± SD: 0.99±0.19 vs. 0.91±0.13 cm/s; P=0.121). TS patients showed, compared to controls, a significantly higher value in the A peak velocity (mean ± SD: 0.69±0.18 vs. 0.54±0.12 cm/s; P=0.002) while displaying a significantly lower ratio E/A (mean ± SD: 1.49±0.33 vs. 1.78±0.45; P=0.009).
Left ventricular systolic deformation
No significant differences in GLPS_A2C (mean ± SD: −18.97%±3.68% vs. −19.21%±2.74%; P=0.809), GLPS_LAX (mean ± SD: −16.45%±4.17% vs. −17.72%±2.86%; P=0.242), GLPS_A4C (mean ± SD: −17.40%±3.05% vs. −17.53%±2.70%; P=0.878) and GLPS_AVG (mean ± SD: −17.61%±3.22% vs. −18.16%±2.18%; P=0.506) were discovered between TS patients and controls.
M-Mode of the abdominal aorta
Abdominal aortic strain assessed by M-Mode was, compared with controls, significantly lower in TS patients (mean ± SD: 14.56%±6.97% vs. 19.74%±9.20%; P=0.040). Arterial distensibility evaluated by M-Mode showed no significant difference between TS and control group (mean ± SD: 6.49±3.45 vs. 8.44±3.56 mmHg−1×10−3; P=0.055).
2DST of the abdominal aorta
Compared with controls, TS patients showed significantly lower peak circumferential strain values in each abdominal aortic layer and a significantly lower arterial distensibility. The results of abdominal aortic 2DST are summarized in Table 3. After adjusting peak circumferential strain values to Dmax, TS patients still displayed significantly lower strain values in AAO-SENDO/Dmax (median, minimum/maximum: 0.70%, 0.20%/2.06% vs. 0.92%, 0.33%/1.89% per mm; P=0.035) and AAO-SMESO/Dmax (mean ± SD: 0.46%±0.22% vs. 0.62%±0.24% per mm; P=0.020). No significant difference was found between TS patients and control subjects in AAO-SEPI/Dmax (mean ± SD: 0.33%±0.16% vs. 0.42%±0.20% per mm; P=0.055).
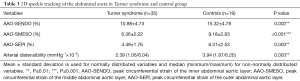

Full table
Correlation between abdominal aortic strain and left ventricular diastolic function
No significant correlation was found between M-Mode assessed abdominal aortic strain and the ratio E/A (r=0.151; P=0.275). A significant positive correlation between the peak circumferential strain of each abdominal aortic layer and the ratio E/A was detected (AAO-SENDO and E/A: r=0.475, P<0.001; AAO-SMESO and E/A: r=0.504, P<0.001; AAO-SEPI and E/A: r=0.393, P=0.003).
Correlation between heart rate and arterial distensibility
Heart rate correlated significantly negative with 2DST assessed arterial distensibility (r=−0.366; P=0.007). No significant correlation was found between heart rate and M-Mode assessed arterial distensibility (r=−0.002; P=0.988).
Correlation between arterial distensibility and oscillometric assessed pulse wave velocity
Of note, PWV was not tracked in three control subjects. No significant difference was observed in PWV between TS patients and controls (median, minimum/maximum: 4.80, 3.80/6.90 vs. 4.75, 3.90/6.50 m/s; P=0.684). No significant correlation was detected between M-Mode assessed arterial distensibility and pulse wave velocity (r=−0.248; P=0.080). A significant negative correlation between 2DST assessed arterial distensibility and pulse wave velocity was discovered (r=−0.491; P<0.001).
Intra- and interobserver variability of abdominal aortic 2DST
Intra- and interobserver variability for each abdominal aortic layer is summarized in Table 4.
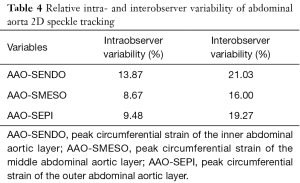
Full table
Discussion
Functional vascular impairments in TS patients
In our study, we prospectively examined the arterial stiffness of the abdominal aorta through M-Mode and 2DST in 35 TS patients and 19 healthy controls. We could demonstrate that TS patients showed, compared with age matched controls, significantly lower abdominal aortic strain values in both sonographic methods, indicating higher arterial stiffness and thus possible functional vascular impairments of the abdominal aorta. Recent studies could display similar findings of increased arterial stiffness in TS patients (7-9,19). The elevated arterial stiffness in TS can be partly explained through associated cardiovascular and cardiometabolic risk factors like diabetes, arterial hypertension, lipid anomalies and excess weight (2,3,20). Those risk factors which are commonly seen in TS patients increase the risk of developing arteriosclerosis, even in young age (2,3). In addition, TS might be associated with intrinsic factors that negatively impact aortic wall elasticity and thus cause its early stiffening (9). To the extent of our knowledge, the negative impact of an elevated heart rate on arterial distensibility in TS patients has not been described yet. In the present study, we demonstrated a correlation between aortic stiffness and heart rate. Though the correlation is weak, it would be interesting to investigate in further studies whether these patients may benefit from medication that lowers heart rate such as beta-blockers or funny channel inhibitors such as “Ivabradine”.
Non-invasive techniques to assess arterial stiffness
Even though magnetic resonance imaging is considered to be the gold standard to measure aortic arterial stiffness, it remains cost expensive and is not ubiquitously available. To the best of our knowledge, this is the first study that utilizes 2DST to evaluate arterial stiffness in TS patients. The benefits of this approach are, as mentioned in the introduction, non-invasiveness and angle independency. Moreover, this technique is relatively time and cost efficient.
In the present study, arterial stiffness was additionally evaluated by measuring PWV through an oscillometric device. Using this well recognized method, no significant difference in PWV and thus arterial stiffness was observed between TS patients and controls. The median PWV value was in the normal range of reference percentiles as defined by Elmenhorst et al. for the TS and the control group (17). The discrepancies between PWV and ultrasound-assessed arterial stiffness could be due to the relatively small sample size of this study. To visualize possible differences in PWV between TS patients and control subjects, larger study cohorts might be necessary. 2DST assessed arterial distensibility correlated significantly with oscillometric determined pulse wave velocity, which is a well-recognized method to evaluate arterial stiffness. In contrast, no correlation was found between M-Mode assessed arterial distensibility and pulse wave velocity. This might be due to the one-dimensional image acquisition of M-Mode which leads to a possibly less accurate arterial stiffness measurement. Differences in arterial stiffness were, compared to M-Mode echocardiography, more pronounced between TS and control group using 2DST of the abdominal aorta. This might suggest that 2DST assesses arterial stiffness more precisely than M-Mode echocardiography.
The regular and precise screening of arterial stiffness in TS is important. First, to estimate an individual’s cardiovascular risk, and second, to monitor the treatment success of the above mentioned cardiovascular and cardiometabolic risk factors on the vascular system. Therefore, 2DST of the abdominal aorta might provide additional diagnostic value for the current vascular screening in TS; particularly for cardiologists that are using 2DST for myocardial evaluation during echocardiographic routine examinations.
Arterial stiffness and left ventricular diastolic function
In the present study, we could demonstrate a left ventricular diastolic dysfunction in TS patients visualized by the ratio E/A. In contrast, left ventricular dimensions and left ventricular systolic deformation, which was assessed through 2DST echocardiography, did not differ significantly between both groups. This may indicate that diastolic dysfunction precedes the systolic one in this cohort. Mottram et al. support this hypothesis by illustrating the negative impact of a high arterial stiffness on diastolic cardiac function (21). In the present study we found a significant positive correlation between the peak circumferential strain of each abdominal aortic layer and left ventricular diastolic function, suggesting that a low aortic strain and therefore a high arterial stiffness has a negative effect on left ventricular diastolic function. Out of all three peak circumferential strain values, AAO-SMESO correlated the strongest with the ratio E/A. We assume that speckles of the middle abdominal aortic layer might track the aortic wall more precisely. Speckles of the inner layer might be affected by noise from the blood pool, while speckles of the outer layer might be affected by tracking para-aortic structures.
Andersen et al. demonstrated that diastolic dysfunction exists in more than a quarter of normotensive, non-obese and insulin sensitive TS subjects (22). Therefore, the management of arterial stiffness should be considered an important factor when facing decreased left ventricular diastolic function in patients with TS. Antihypertensive drugs like ACE inhibitors, calcium channel blockers or mineralocorticoid receptor antagonists might be beneficial to decrease arterial stiffness and thus might also improve left ventricular diastolic function in TS patients (23). The increased aortic stiffness is, however, not the only culprit for diastolic function observed frequently among this cohort since the correlation is rather weak. Other factors, beyond the scope of the present study, should be involved in such a process. Interestingly, we found a significantly higher heart rate in TS patients. Other studies have shown similar findings, suggesting that the elevated heart rate in TS subjects is due to sympathetic dysregulation (22,24,25). The impact of higher heart rate on the diastolic function has been previously reported (26,27). An increase in heart rate results in a decrease of early mitral inflow velocity (E) and an expansion of the A-wave, resulting in a lower ratio E/A (26). This should be considered when assessing diastolic heart function through Doppler echocardiography in TS patients with a high heart rate.
Limitations
The main limitation of 2DST is the relatively high intra- and interobserver variability that we could observe in this study. The accuracy and consequently the observer variability of 2DST is dependent on the sonographic window and on heart rate. In overweight patients in which image quality is often reduced or in patients with a high heart rate, aortic speckles might not be tracked as accurately, leading to imprecise strain values. Due to insufficient sonographic window and increased heart rate, four TS patients could not be included this study. Moreover, the impact of curvature dependency on measured aortic circumferential strain should be considered when facing patients with suspected variable diameters of the abdominal aorta (28). In such cases, strain values could be corrected to the diameter of the abdominal aorta to reduce curvature dependency. Even after the acquired strain values were adjusted to maximal abdominal aortic diameter in this study, TS patients showed, compared to controls, significantly lower abdominal aortic strain values in AAO-SENDO and AAO-SMESO. Ultimately, 2DST of the abdominal aorta has not been validated in large studies yet using widely accepted arterial stiffness measuring methods like magnetic resonance imaging, computer tomography or applanation tonometry. Furthermore, strain reference values for 2DST of the abdominal aorta have not been established yet. This study was limited by its relatively small amount of control subjects. This makes it difficult to interpret physiological ranges of abdominal aortic strain assessed through 2DST.
Conclusions
Functional vascular impairments of the abdominal aorta associated with TS can be detected using 2DST. In comparison to M-Mode, 2DST of the abdominal aorta might add additional diagnostic value to the current vascular screening in patients with TS. In our study, 2DST of the abdominal aorta was limited by a relatively high observer variability. Further studies must apply 2DST of the vascular system in large cohorts to validate this method and to establish reference values.
Acknowledgments
We would like to thank all study participants and the German Turner Syndrome Association (Turner-Syndrom-Vereinigung Deutschland e.V.) for the interest in our study.
This study was supported by the Competence Network for Congenital Heart Defects, which received funding from the Federal Ministry of Education and Research, Grant Number 01GI0601 [2014], and the German Centre for Cardiovascular Research, Grant Number 81X2800112 [2015].
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: This study was approved by the Ethics Committee of the Ärztekammer des Saarlandes (State Chamber of Physicians of the German federal state of Saarland) (approval statement No. 07/18). Prior written informed consent was obtained from all patients or the parents or legal guardians of patients under legal age.
References
- Sybert VP, McCauley E. Turner's syndrome. N Engl J Med 2004;351:1227-38. [Crossref] [PubMed]
- Mavinkurve M, O'Gorman CS. Cardiometabolic and vascular risks in young and adolescent girls with Turner syndrome. BBA Clin 2015;3:304-9. [Crossref] [PubMed]
- Gravholt CH, Andersen NH, Conway GS, et al. Clinical practice guidelines for the care of girls and women with Turner syndrome: proceedings from the 2016 Cincinnati International Turner Syndrome Meeting. Eur J Endocrinol 2017;177:G1-70. [Crossref] [PubMed]
- Mazzanti L, Cacciari E. Congenital heart disease in patients with Turner’s syndrome. J Pediatr 1998;133:688-92. [Crossref] [PubMed]
- Schoemaker MJ, Swerdlow AJ, Higgins CD, et al. Mortality in women with turner syndrome in Great Britain: a national cohort study. J Clin Endocrinol Metab 2008;93:4735-42. [Crossref] [PubMed]
- Mitchell GF, Hwang SJ, Vasan RS, et al. Arterial stiffness and cardiovascular events: the Framingham Heart Study. Circulation 2010;121:505-11. [Crossref] [PubMed]
- An HS, Baek JS, Kim GB, et al. Impaired Vascular Function of the Aorta in Adolescents with Turner Syndrome. Pediatr Cardiol 2017;38:20-6. [Crossref] [PubMed]
- Uçar A, Öz F, Baş F, et al. Increased arterial stiffness in young normotensive patients with Turner syndrome: associations with vascular biomarkers. Clin Endocrinol (Oxf) 2015;82:719-27. [Crossref] [PubMed]
- De Groote K, Devos D, van Herck K, et al. Increased aortic stiffness in prepubertal girls with Turner syndrome. J Cardiol 2017;69:201-7. [Crossref] [PubMed]
- Oishi Y, Mizuguchi Y, Miyoshi H, et al. A novel approach to assess aortic stiffness related to changes in aging using a two-dimensional strain imaging. Echocardiography 2008;25:941-5. [Crossref] [PubMed]
- Teixeira R, Vieira MJ, Gonçalves A, et al. Ultrasonographic vascular mechanics to assess arterial stiffness: a review. Eur Heart J Cardiovasc Imaging 2016;17:233-46. [Crossref] [PubMed]
- Mosteller RD. Simplified calculation of body-surface area. N Engl J Med 1987;317:1098. [Crossref] [PubMed]
- Pettersen MD, Du W, Skeens ME, et al. Regression equations for calculation of z scores of cardiac structures in a large cohort of healthy infants, children, and adolescents: an echocardiographic study. J Am Soc Echocardiogr 2008;21:922-34. [Crossref] [PubMed]
- Cho JY, Kim KH. Evaluation of Arterial Stiffness by Echocardiography: Methodological Aspects. Chonnam Med J 2016;52:101-6. [Crossref] [PubMed]
- Feistritzer HJ, Klug G, Reinstadler SJ, et al. Oscillometric analysis compared with cardiac magnetic resonance for the assessment of aortic pulse wave velocity in patients with myocardial infarction. J Hypertens 2016;34:1746-51. [Crossref] [PubMed]
- Hametner B, Wassertheurer S, Kropf J, et al. Oscillometric estimation of aortic pulse wave velocity: comparison with intra-aortic catheter measurements. Blood Press Monit 2013;18:173-6. [Crossref] [PubMed]
- Elmenhorst J, Hulpke-Wette M, Barta C, et al. Percentiles for central blood pressure and pulse wave velocity in children and adolescents recorded with an oscillometric device. Atherosclerosis 2015;238:9-16. [Crossref] [PubMed]
- Aristizábal-Ocampo D, Espíndola-Fernández D, Gallo-Villegas J. Pulse wave velocity reference values in 3,160 adults referred to a hypertension clinic for 24-hour ambulatory blood pressure monitoring. Clin Exp Hypertens 2018. [Epub ahead of print]. [PubMed]
- Schäfer M, Browne LP, Truong U, et al. Aortic stiffness in adolescent Turner and Marfan syndrome patients. Eur J Cardiothorac Surg 2018;54:926-32. [Crossref] [PubMed]
- Palombo C, Kozakova M. Arterial stiffness, atherosclerosis and cardiovascular risk: Pathophysiologic mechanisms and emerging clinical indications. Vascul Pharmacol 2016;77:1-7. [Crossref] [PubMed]
- Mottram PM, Haluska BA, Leano R, et al. Relation of arterial stiffness to diastolic dysfunction in hypertensive heart disease. Heart 2005;91:1551-6. [Crossref] [PubMed]
- Andersen NH, Hjerrild BE, Sørensen K, et al. Subclinical left ventricular dysfunction in normotensive women with Turner's syndrome. Heart 2006;92:1516-7. [Crossref] [PubMed]
- Dudenbostel T, Glasser SP. Effects of antihypertensive drugs on arterial stiffness. Cardiol Rev 2012;20:259-63. [Crossref] [PubMed]
- Gravholt CH. Turner syndrome and the heart: cardiovascular complications and treatment strategies. Am J Cardiovasc Drugs 2002;2:401-13. [Crossref] [PubMed]
- Zuckerman-Levin N, Zinder O, Greenberg A, et al. Physiological and catecholamine response to sympathetic stimulation in turner syndrome. Clin Endocrinol (Oxf) 2006;64:410-5. [Crossref] [PubMed]
- Burns AT, Connelly KA, La Gerche A, et al. Effect of heart rate on tissue Doppler measures of diastolic function. Echocardiography 2007;24:697-701. [Crossref] [PubMed]
- Johnson MC. Diastolic function and tachycardia in hypertensive children. Am J Hypertens 1999;12:1009-14. [Crossref] [PubMed]
- Spriestersbach H, Oh-Icí D, Schmitt B, et al. The influence of the region of interest width on two-dimensional speckle tracking-based measurements of strain and strain rate. Echocardiography 2015;32:89-95. [Crossref] [PubMed]


